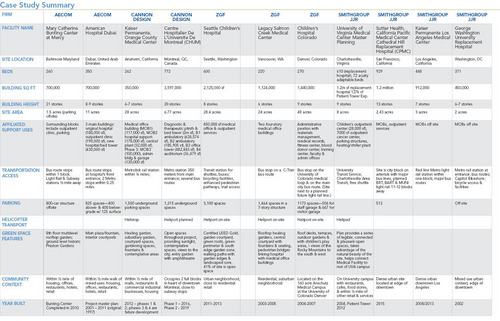
Hospital case studies point the way for Prince George’s

Image from ZGF.
What’s the difference between a hospital that’s a springboard for economic development, and one that’s not living up to its potential? Answer: Design, location, and connectivity. Local groups compiled a set of case studies to point the way as Prince George’s County moves forward with its proposed Regional Medical Center.
The new hospital is an important healthcare facility for the county, and as an employer of 2,000 workers, it can also catalyze economic development in an area where new investment has lagged.
Hospital officials are rumored to be interested in a sprawling 80-120 acre suburban-style site away from Metro, likely the old Landover Mall site. The sponsors of the case studies hope that these examples of great hospitals, designed by leading architectural firms, can help decision-makers understand the benefits of a more mixed-use, compact and transit-oriented site.
Envision Prince George’s Community Action Team for Transit-Oriented Development, the Coalition for Smarter Growth, and American Institute of Architects Potomac Valley collected the design case studies. They provide examples of mid- to large-scale hospitals with footprints of 1.5-48 acres. In fact, larger hospitals (measured in number of beds) are at the lower end of this range of acres, while the smaller hospitals tended to occupy more land area.
While Prince George’s continues to pursue additional federal offices (like the new FBI headquarters), a new $600 million medical center could be one of the best opportunities to jump-start transit-oriented development at one of the county’s 15 underutilized Metro stations.
In contrast to courting federal agencies, the state and county control the decision about where to locate and how to design a new medical center. Not encumbered with stringent federal security requirements, a regional medical center offers a better opportunity to connect to surrounding uses and fuel spinoff economic activity than an FBI or Homeland Security building.
Why a smaller, urban footprint?
Hospitals must plan for growth, and a working “rule of thumb” for traditional suburban or rural 200-bed hospitals (similar in size to the Prince George’s facility) is a minimum of 40 acres. This footprint provides a suburban or rural site with room for the initial building, associated drop-offs, parking, and room for future growth. Growth is common in medical facilities, whether for outpatient clinics, specialty centers, or the hospital itself.
Hospitals in a more urban context plan for similar growth, but within sites that are typically 10 acres or less. This smaller footprint offers several benefits over a suburban medical campus. Connecting a hospital center to a larger mixed-use environment where people can work, shop, and live helps attract and retain highly sought-after skilled healthcare workers. By better integrating into the surrounding community, an anchor institution like this can support a vibrant, walkable, thriving new hub.
Designers also point to sustainability benefits from a more urban design and context. A limited footprint disturbs less land and reduces the heat island effect. Placing a more compact medical center in an urban hub also allows for more environmentally-friendly transportation choices with frequent transit service, and walk and bicycle options for short trips. Driving and parking will remain an important mode of access, but a more urban hospital allows for lower parking supplies, greater access for those who do not have a car, and the choice to take some trips on foot or by bicycle.
While a footprint of 10 acres may seem small compared to a suburban campus of 40 acres or more, hospital complexes around the country and beyond are developing successful, busy hospitals on sites as small as a few acres.
The just-released case studies of 11 successful moderate to small-footprint hospitals of comparable size to the planned Prince George’s regional medical center share 3 common success factors: access, flexibility for future growth, and a connection to the surrounding environment.
Success factor: Access
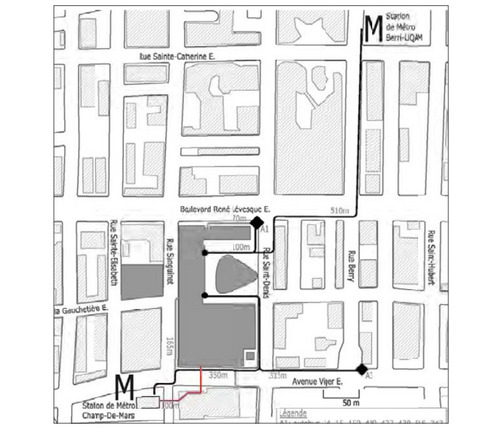
An important factor for any healthcare facility is convenient and easy access to and from the site. High-quality public transportation, stores and services, and housing within walking distance create opportunities for staff and visitors to get outside the hospital while still being nearby, and enable some to come and go without having a car.
Several of the examples in the report show major hospitals that are integrated into city blocks. Hospital staff and visitors have easy access to a local services and transit options. For example, the Kaiser Permanente Los Angeles Medical Center is a 448-bed hospital, 7 stories tall situated on 3 acres of land. Within a block is the Red line light rail station and major bus routes.
Closer to home, the 6-7 story, 371-bed George Washington University Hospital occupies 2 acres. The front door of GWU Hospital opens onto the busy entrance of the Foggy Bottom Metrorail station and is embedded in a thriving urban district that mixes health, university, private office, retail and housing uses in a highly walkable, transit-accessible environment.
Medical facilities woven into the fabric of a larger mixed-use district served by transit can have an advantage when competing for medical professionals who desire to be in a lively, diverse place, and need flexibility with their commutes in a two-worker household.
Success factor: Flexibility for future growth
While suburban hospitals are typically designed with extra acreage to accommodate future growth, urban medical centers can anticipate similar growth, but plan smartly within a more constrained footprint.
Planning a smaller-footprint facility guides planners to take into account their overall surroundings, making better use of pedestrian connections to the surrounding community and supporting services. In the case of both the vertical high rise addition to Mercy Medical Center in Baltimore, with the 260-bed Bunting Center inpatient hospital on 1.5 acres, and the 350-bed American Hospital Dubai campus on 11 acres, planning for growth accounted for the sites’ larger surroundings.
The hospital designers from AECOM point out that an urban design and location provides significant advantages in offering the ability to walk to a nearby restaurant to avoid yet another meal at the hospital cafeteria or the convenience of staying at a nearby hotel for someone visiting a sick relative.
Success factor: Connection to green spaces
Numerous studies show that access to outdoor places and views of green spaces create a state-of-the-art healing environment. But urban hospitals don’t need to concede healing green features to their suburban and rural counterparts. Roof gardens, courtyards, and natural light are all achievable in small-footprint hospital centers.
The centerpiece of the Bunting Center at Mercy Hospital healing environment is a multilevel roof garden, accessible on various floors and overlooked by room occupants above the midway point along the rise of the building. The 9th floor garden offers direct access from the ICU waiting room.
On the 28 acre campus of the 600-bed Seattle Children’s Hospital, 41% of the campus is dedicated as open space. Pedestrian paths are provided throughout the facility to promote walking and offer outdoor connections.
Innovative design and urban context show the possibilities
The 11 case studies offer examples of innovative architectural design, connectivity to the surrounding context, access to transit, green features and compact footprints. These features highlight how a regional medical center for Prince George’s and Southern Maryland could establish a new leading healthcare facility that not only attracts the staff and patients it needs to succeed, but fits into a larger district that thrives on the influx of activity.